To the old saying about the inevitability of death and taxes, we should add another: another health crisis linked to COVID-19. As of the end of October, the CDC's official tally of U.S. COVID infections was just under 100 million, but with many positive home test results unreported, the real number is estimated to be several times greater.
Infections, while unfortunate and sometimes deadly, do provide immunity to survivors, but only for a limited time. Natural post-infection and vaccine-induced immunity wane over a period of months, so that a large fraction of the U.S. population remains potentially susceptible to infection.
Reason for concern?
A swarm of new Omicron subvariants is now emerging, and some may be very dangerous. But fewer than 10% of eligible Americans have taken advantage of the new bivalent COVID vaccine boosters, which enhance resistance to all the known Omicron subvariants as well as Omicron's predecessors. Yet, fewer and fewer people are opting to get a booster. This makes a winter surge likely, and it could get scary.
Most people who have had COVID have recovered within a few days or, at most, weeks, but some, even those who had mild infections, can have persistent, debilitating symptoms that last months or even years.
The most common long COVID symptoms are fatigue, fever, cough and difficulty breathing or shortness of breath. Less common problems are "brain fog," headache, stroke, sleep problems, loss of smell and taste, depression or anxiety; joint or muscle pain; cardiovascular symptoms such as chest pain and palpitations; digestive symptoms; new-onset diabetes; and blood clots in various organs.
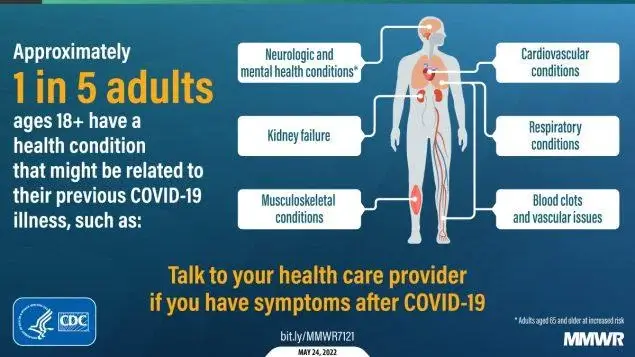
Long COVID occurs in around five percent of those who have been infected. Note that long COVID is persistence of symptoms after acute infection, while the CDC figure in the above graphic refers to the appearance of new conditions sometime after the acute infection
Long Covid causes extended pain and suffering in many millions of Americans and severe symptoms in perhaps a million who are unable to work. Not surprisingly, there are elevated numbers of "excess deaths" — above what are predicted from historical data.
A vaccine still remains the first line of defense. "The best way not to have long COVID is not to have COVID at all," says Leora Horwitz, MD, a professor of population health and medicine at New York University's Grossman School of Medicine. And vaccination lowers the likelihood and severity of infection, as well as of hospitalization and death in those who do become infected.
However, only about two–thirds of Americans have had the primary series of two vaccinations, and the effectiveness of those shots has waned significantly. Only about nine percent have had the updated bivalent booster that offers the strongest protection against known variants.
How much protection do the latest vaccine boosters confer?
A modeling study by the Commonwealth Fund illustrates vividly the importance of greater uptake of the bivalent vaccine booster. It found that if about 54% of Americans will have taken it by the end of this year, by March 31, 2023, some 75,000 deaths would be prevented, about three-quarters of a million hospitalizations averted, and some $44 billion in direct medical costs saved.
The graphic representation of the study's results is striking. The two graphs predict projected seven-day rolling average of COVID-19 hospitalizations (left graph) and deaths (right graph) in the U.S., under different booster vaccination coverage scenarios. They show projected hospitalizations and deaths from COVID-19 with the current rate of COVID bivalent boosters (upper curve), a rate equal to the frequency of flu vaccination last year (approximately 54%, middle curve), and 80% coverage of the bivalent booster (lowest curve).
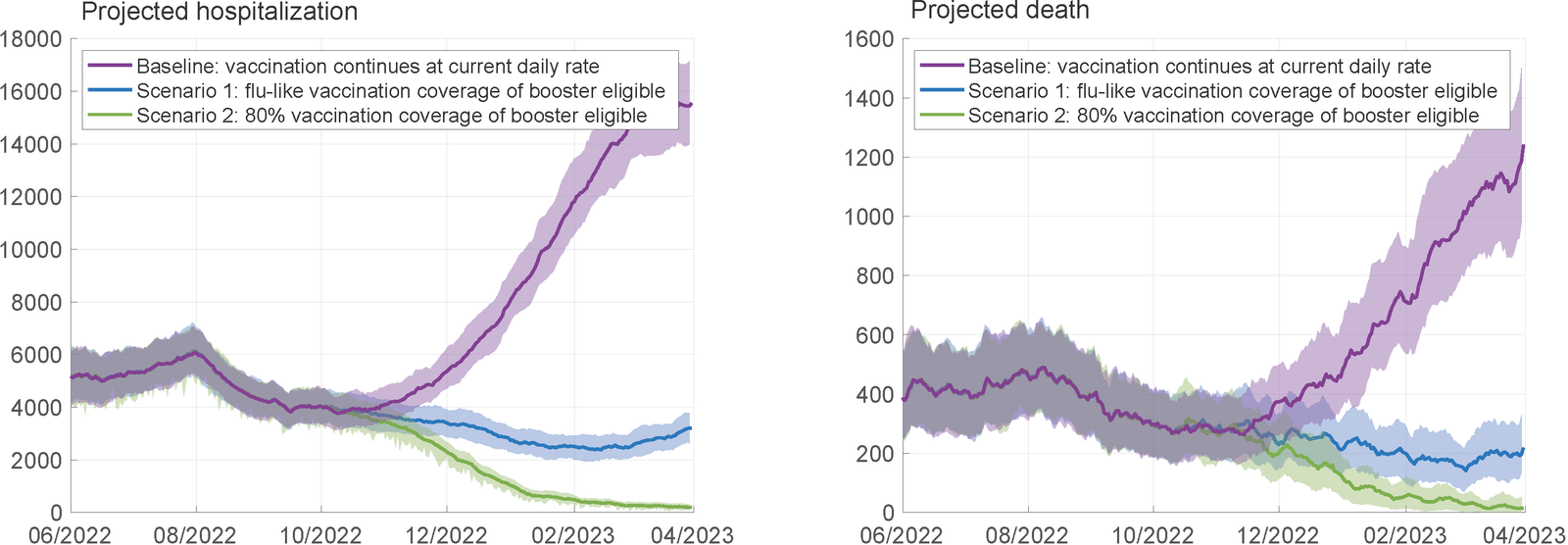
Scenario 1: flu-like vaccination coverage of booster eligible
Scenario 2: 80% vaccination coverage of booster eligible
[Note: In the baseline scenario, vaccination rates are held constant at the average of the daily vaccination rate for August 2022 until the end of March 2023]
The data point to an indisputable conclusion: A full court press to convince skeptical Americans to get the latest COVID booster, and a solid response, could save thousands of lives and billions of dollars.
As shown by the lowest of the curves in both graphs, with 80% uptake of the bivalent booster vaccines (Scenario 1), the U.S. could virtually eliminate hospitalizations (left graph) and deaths (right graph) from COVID by the end of March 2023. Even a relatively modest increase in uptake (the middle curves) would exert a significant effect, but this goal will become more elusive when the federal government's paying for shots ends soon. The out-of-pocket cost to uninsured individuals would then be more than $100.
Another benefit of broader vaccination would be that people who get the COVID-19 vaccine but still develop COVID are at significantly lower risk of symptoms of long COVID or the onset of new illnesses, when compared to those who are not vaccinated.
Over the course of the pandemic, the death rate in the U.S. has been the worst among developed, industrialized, countries. We have safe and effective tools to turn that around, but they are no good if we don't use them.
Henry I. Miller, a physician and molecular biologist, is a Senior Fellow at the Pacific Research Institute. He was the founding director of the Office of Biotechnology at the FDA. Please follow him on Twitter at @henryimiller
John J. Cohrssen is an attorney who has served in several government posts in both the executive and legislative branches of government.

