Many of us in the medical community feel as though we're having one of those dreams in which we're shouting a warning about an impending disaster – a speeding truck about to hit a pedestrian pushing a stroller, for example – but no one seems to hear it.
I'm referring to ever-persisting COVID-19. We are experiencing a perfect storm of circumstances leading to another surge of coronavirus infections, but instead of addressing it by getting ahead of deteriorating circumstances, many politicians, public health officials, and individuals are choosing simply to "move on."
That's not a plan, that's the absence of a plan.
In science, we often return to "first principles" for a solution to a problem. For the COVID-19 pandemic, four such factors help us to predict the future of the pandemic and suggest a strategy.
- First is the nature of the virus itself – its transmissibility, virulence, and propensity to mutate.
- Second is the state of immunity in potential targets of the virus – that is, the public.
- Third is the availability of drugs to treat and mitigate the effects of the infection in infected persons.
- Fourth is behavioral – how intensely people apply non-pharmaceutical interventions to prevent becoming infected.
Let's take them one at a time.
Evolution of the SARS-CoV-2 virus
First, much of the U.S. is experiencing a new wave of COVID-19 infections caused by a new Omicron variant called BA.2.12.1, which is significantly more transmissible – that is, infectious – than any of its predecessors, and is now the predominant variant in this country.
The confirmed case count daily average in early June was just over 100,000, which we know is a significant undercount because many tests are now done at home, positive results are not routinely reported to authorities, and many asymptomatic cases are not tested at all. The true number is probably closer to half a million per day. COVID-19 hospitalizations are trending upwards, as are nationwide levels of coronavirus in wastewater, according to the CDC's "National Wastewater Surveillance System." On May 30th, 19% of the surveillance sites reported that virus levels were up 10-99% over the previous 15 days, while 35% had jumped 100% or more. This is a bad portent.
In fact, surges are already being reported in much of the country. The case load in Hawaii, which had largely contained COVID, surged for the 10th week in a row, crippling hospitals. Some 800 frontline caregivers called in sick over the past week due to COVID-19 infections.
There are many reasons for the surges. Many people believe that infections are almost universally mild, and that, in any case, it's virtually inevitable that they'll eventually become infected. Another contributing factor is the lifting of mask and vaccine mandates by businesses, including airlines, restaurants, supermarkets, and other stores. Whatever the reason, this indifference is worrisome, because every infection gives rise to viral replication and the appearance of more mutants.
Also, according to a large new study by the CDC, one in five adult survivors of COVID-19 under the age of 65 in the U.S. has experienced at least one health condition that could be considered "long COVID," a broad spectrum of signs and symptoms related to many organ systems that can last for months or longer following the initial infection.
At the same time, the CDC continues to propagate the fantasy that community levels of infection are very low, although the important data indicate that transmission is very high throughout most of the country. Irresponsibly feeding the myth that the pandemic is over – which, of course, is precisely what everyone wants to believe – induces many people to lower their guard. The evidence of that is the many unmasked people now in stores, airports, airplanes, religious services, and other gatherings.
Immunity in the population
Immunity to Omicron and its variants is somewhere between suboptimal and dismal. For one thing, the U.S. population is under-vaccinated and under-boosted, and immunity – from either natural infection or vaccination – wanes with time. While California has achieved more than 70 percent of its population with full vaccine coverage, a large number of states — including Missouri, Georgia, Arkansas, Alabama, Wyoming, Indiana — have barely reached 50 percent.
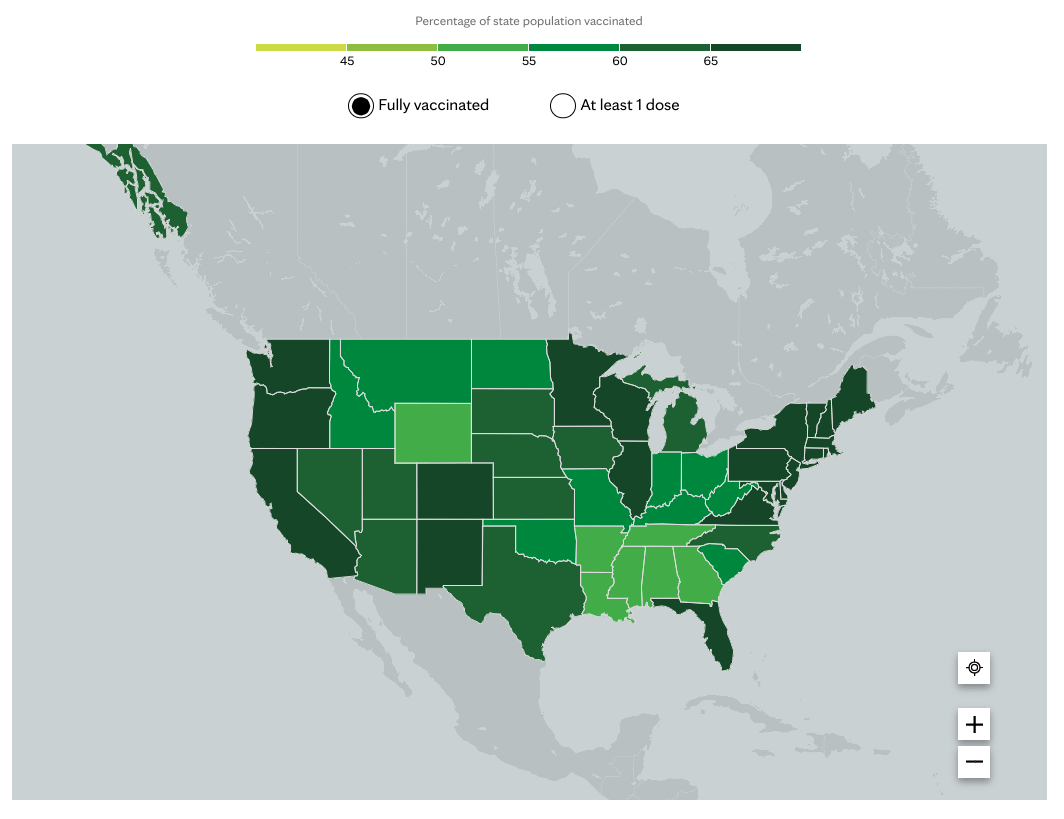
BA.2.12.1, the currently dominant variant of Omicron in the U.S., is quite distinct from earlier Omicron variants BA.1 and BA.2, as are the other newer Omicron subvariants, BA.4 and BA.5, which were recently designated "variants of concern" by the European Centre for Disease Prevention and Control. All of these are better able than earlier SARS-CoV-2 variants to evade immunity from natural infection or immunization with existing vaccines. That's why, increasingly, we are seeing "breakthrough" infections in people who have been vaccinated and even boosted. Fortunately, new versions of the vaccines designed to protect against Omicron variants are in development.
Drug treatments
We now have several good oral drugs to treat COVID-19, but none is perfect. Molnupiravir is only about 30% effective and Paxlovid, although about 90% effective in the clinical trials, has potentially dangerous drug-drug interactions with many commonly prescribed medicines. Moreover, in a small number of patients we're seeing "Paxlovid rebound" — a return of their COVID symptoms a few days to a couple of weeks after initial recovery. The symptoms are usually mild and there have been no reports of severe disease during the rebound, but the cause of the phenomenon is as yet unknown.
Individuals' behavior
Here is the thorniest factor: Americans are not behaving well. Aside from rejecting vaccination in shocking numbers, many have discarded their masks, even in high-risk settings. And they are increasingly putting themselves in those situations, such as class trips, parties, concerts, conferences, airplane flights, and cruises. Even medical meetings are not immune. For example, a number of attendees at the annual meeting of the Society for Academic Emergency Medicine (SAEM), May 10-13, tested positive for COVID-19 after the event which brought thousands to a hotel in New Orleans amid an uptick in cases and hospitalizations nationwide. COVID-19 vaccines were required, but masks were only "encouraged," and few wore them in the tightly packed indoor space. If Emergency Room docs won't take proper precautions, how can we expect the general public to do so?
As Scripps Research Dr. Eric Topol wrote recently, "we absolutely need an aggressive stance to get ahead of the virus — for the first time since the pandemic began — instead of surrendering. That makes setting priorities, funding, and the realization, unfortunately, that the pandemic is far from over." Very simply, we need judiciously targeted mask and vaccine mandates and widespread testing to, once again, flatten the curve of infections.
"Humans naturally get tired," Dr. Topol emphasized, "but they shouldn't be foolish or outsmarted by a virus."
Dr. Henry Miller, a physician and molecular biologist, was the founding director of the FDA's Office of Biotechnology and a Consulting Professor at Stanford University's Institute for International Studies. Find his articles at henrymillermd.org

